To take a closer look at access to care, PPIC has created an interactive, California Critical Care during COVID-19.
To reduce community spread of COVID-19, California has instituted statewide guidance to shelter in place until further notice, and to practice social distancing when leaving home for approved activities such as grocery shopping or exercise. Because COVID-19 is novel, no vaccine is available and no one has preexisting immunity. However, individuals are not equally at risk, and there are several known sources of vulnerability.
There are Californians at elevated risk of exposure to the coronavirus. For some, this risk is due to the nature of their work, as is the case for physicians, nurses, and other front-line medical staff. For others, such as California’s approximately 115,000 prisoners and 150,000 homeless individuals, living conditions pose serious challenges to social distancing. And being over 60 or having an underlying health condition makes over one-third of California’s adults especially vulnerable to serious or fatal complications—this estimate does not include undiagnosed medical conditions, which puts the actual figure higher.
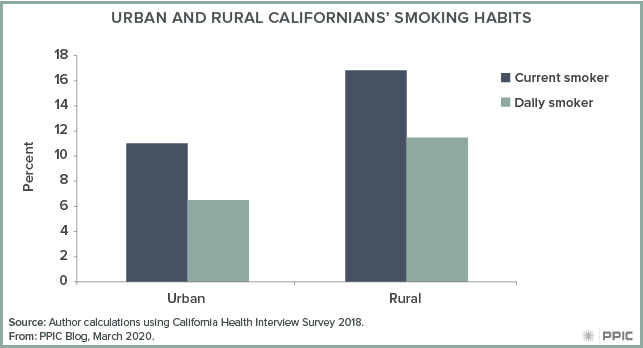
Californians in the state’s 21 rural counties may have lower exposure to the coronavirus because of the relative ease of social distancing. These individuals, who make up over 837,000 residents, may face significant challenges if they do contract the coronavirus. California’s rural adults are more likely to smoke than urban ones (16.8% versus 11.0%) (California Health Interview Survey 2018), and smoking is suspected to put coronavirus patients at higher risk of complications because it is known to damage lung health.
Rural residents often have to travel farther to access critical care resources. This is especially concerning for the large numbers of elderly Californians who are low income, geographically isolated, or living alone in the state’s rural areas (California Department of Aging 2019).





