Summary
California’s senior population is entering a period of rapid growth. By 2030, as the Baby Boom generation reaches retirement age, the over-65 population will grow by four million people. It will also become much more racially and ethnically diverse, with the fastest growth among Latinos and Asians. Many more seniors are likely to be single and/or childless’suggesting an increased number of people living alone. All of these changes will have a significant impact on senior support services.
We project that by 2030 slightly more than one million seniors will require some assistance with self-care, and that the demand for nursing home care will begin to increase after decades of decline. These changes will have direct budget implications for the Medi-Cal and In-Home Supportive Services (IHSS) programs, both of which pay for care and services for low-income seniors. The state will need additional resources, including nursing care facilities and health care professionals, especially those who provide home- and community-based services. California’s community college system will be critical in training workers to meet the state’s health care workforce needs for the growing and changing senior population.
Introduction
California’s senior population will grow substantially by 2030, when the youngest Baby Boomers hit retirement age. This report highlights how this population is growing and changing. We also project some of the potential age-related needs this population will face-in particular, the number of seniors who will have trouble caring for themselves and the number who will require full-time nursing home care.
As people age, they tend to require more medical care. They are increasingly likely to have trouble living alone’some will need home- or community-based health services, others will move into assisted living, and still others, mainly those with the most serious self-care limitations, will enter nursing homes. The spectrum of age-related needs points to an increased demand for a variety of support workers, from home health aides to nurses and doctors. While care requirements for California’s aging population will continue to evolve past 2030, the estimates in this report provide a useful starting point for the state to plan for changes in the demand for home-based care and nursing home facilities.
Changes in the senior population
Over the next two decades, California’s over-65 population will nearly double, clearly indicating an increased demand for health and support services. This population will also become more racially and ethnically diverse, signaling a growing need for culturally competent care-that is, care that respects the beliefs and responds to the linguistic needs of seniors from diverse backgrounds. In addition, the senior population in 2030 will have more single and/or childless adults than it does today, suggesting an increased number of people living alone. This particular shift is likely to have a significant impact on senior support services, since on average, people living alone as they age are more likely to need either home health care or nursing home care. Taken together, all of these changes point to a new and evolving landscape for senior care in the state.
California’s over-65 population is expected to be 87 percent higher in 2030 than in 2012, an increase of more than four million people (Figure 1).1 This group will grow much faster than the rest of the population, rising from 12 percent in 2012 to 19 percent in 2030. Because of this faster growth, there will be fewer adults of prime working age relative to the senior population.2 As a result, a greater share of the state’s human and economic resources will be used to provide health care and other types of support for this group.
The first Baby Boomers began hitting retirement age in 2011, and the youngest will turn 65 in 2029. Figure 1 shows historical and projected levels of the state’s senior population broken down into age groups. In 2030 most seniors will be relatively young, between age 65 and 75. However, beginning in 2020 the fastest growth will occur among seniors age 75 and older. By 2030, the over-85 population will have grown considerably, increasing 61 percent (around 400,000 people) from 2012.
Figure 1. California’s senior population will nearly double by 2030
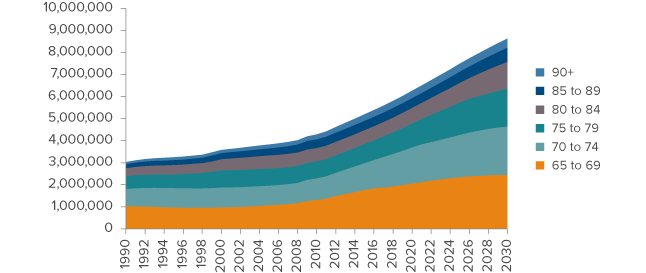
SOURCE: State of California, Department of Finance, State and County Population Projections by Race/Ethnicity, Sex, and Age 2010-2060, Sacramento, California, December 2014.
NOTE: See Technical Appendix A for detailed tables and Technical Appendix B for data and methods used to generate the projections.
The number of seniors in every major racial/ethnic group will increase by 2030 (Figure 2). Whites will remain the largest group and are projected to grow by 53 percent (1.5 million people). However, the fastest rates of growth will occur among nonwhite populations, especially Latinos (170%, or 1,430,000 people) and Asians (118% or 765,000 people). The African American senior population will increase by 96 percent, or 230,000 people.
Because Latino and Asian senior populations are growing so quickly, they will make up an increasing share of the total over-65 population going forward (Figure 2). Since 1990, there has been a steady decline in the percent of seniors who are white, and by 2030 that fraction is expected to dip to just below 50 percent. At that point, no ethnic group will constitute a majority of the senior population. Latinos will have increased from 18 percent in 2012 to 26 percent by 2030; Asians will grow from 14 percent to 16 percent. The fraction of seniors who are African American will hold constant at 5 percent.
Figure 2. California will see strong growth for seniors in every ethnic group
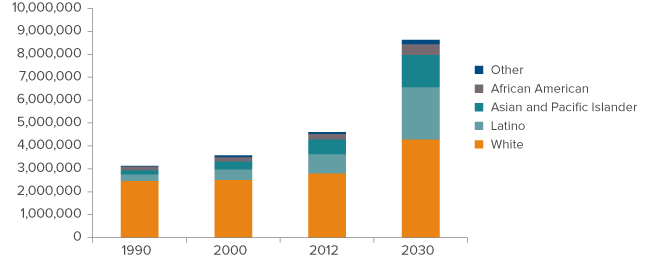
SOURCE: California Department of Finance.
NOTE: See Technical Appendix A for detailed tables.
Family structures in this age group will also change considerably-in particular, marital status will look quite different among seniors in 2030 than it does today (Figure 3). The fastest projected rates of growth are among the divorced/separated and never married groups. Between 2012 and 2030, the number of married people over age 65 will increase by 75 percent-but the number who are divorced or separated will increase by 115 percent, and the number who are never married will increase by 210 percent.
Figure 3. More seniors will be divorced/separated or have never married
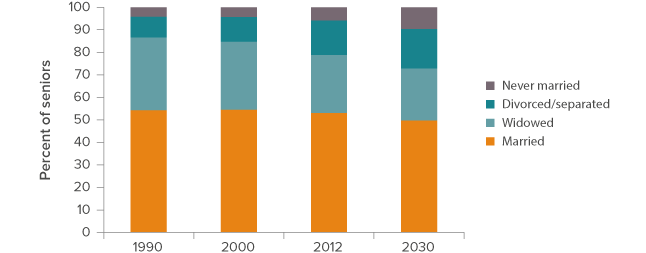
SOURCE: Author calculations based on the American Community Survey and Decennial Census.
NOTE: See Technical Appendix A for detailed tables and Technical Appendix B for data and methods used to generate the projections.
Another significant change will be in the number of seniors who have children. Those who have never been married are much less likely to have children than those who have been married at some point.3 As a result, seniors in the future will be more likely to be childless than those today (Table 1). In 2012, just 12 percent of 75-year-old women had no children. We project that by 2030, nearly 20 percent will be childless.4 Since we know that adult children often provide care for their senior parents, these projections suggest that alternative non-family sources of care will become more common in the future.5
Changes in the need for support services
In the previous section, we established that by 2030, California’s senior population will grow significantly and become more racially and ethnically diverse. In addition, more seniors are likely to live alone, without family members to care for them. In light of these shifts, California policymakers should be considering the kinds of resources that will best address the needs of this changing population. Many seniors will prefer to use services that allow them to remain in their homes. Assisted living facilities provide a range of services with activities of daily living and some medical support for seniors or people with disabilities. For those needing the highest level of care, nursing homes are likely to play an important role-for both long- and short-term care (such as post-surgery recovery). Among the options for seniors requiring some assistance with daily living, nursing homes are by far the most expensive. In this section, we offer a brief overview of the likelihood of needing some sort of care, focusing particularly on potential changes in the need for nursing home care.6
Figure 4. The number of seniors facing difficulties with self care will almost double
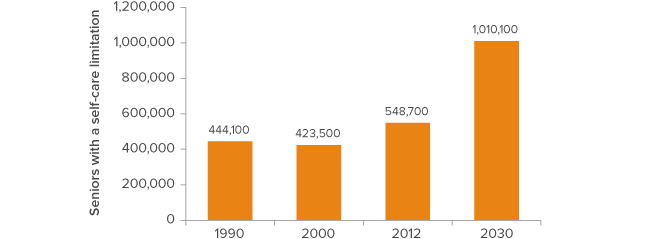
SOURCE: ACS and Decennial Census and author calculations.
NOTE: See Technical Appendix A for detailed tables and Technical Appendix B for data and methods used to generate the projections.
We begin by estimating the number of people who will have difficulty caring for themselves.7 The people in this category have a wide range of needs, from transportation and cleaning services to help with basic tasks such as bathing or eating. The strongest predictors of self-care difficulties are age and marital status, with older seniors and never-married seniors much more likely to experience some type of limitation.8 We project that there will be slightly more than one million seniors with self-care limitations in 2030 (Figure 4).9 This represents an 88 percent increase over 2012 population levels, about the same as the overall increase in the senior population. The vast majority of these seniors-more than 900,000-will not be living in nursing homes.
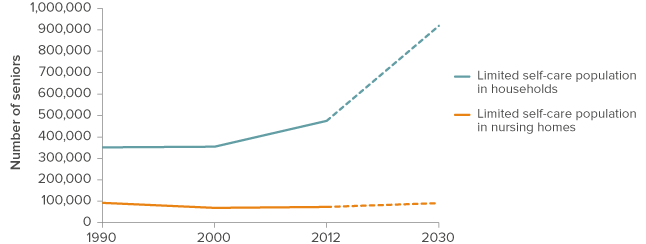
Figure 5. Most seniors with self-care difficulties will be living at home
SOURCE: ACS and Decennial Census and author calculations.
NOTE: See Technical Appendix A for detailed tables and Technical Appendix B for data and methods used to generate the projections.
What about those needing nursing home care? Our projections suggest that these numbers will grow more slowly than the overall senior population. We find that, based on historical trends and future population projections, slightly more than 106,000 people will need nursing home care in 2030 (Figure 5). This represents a 16 percent increase over the 91,500 who were in nursing homes in 2012. These projections assume a continued decline in the rate of reliance upon nursing homes; they also assume that the general preference for living at home and relying on support services will continue to increase.10 However, if the likelihood of living in a nursing home remains the same over time, then the number of seniors in nursing homes will exceed 150,000 by 2030.
Who is most likely to need nursing home care?11 The single most important predictor is having difficulty with daily activities-in fact, our findings suggest that age alone is becoming a less significant factor than self-care limitations. Other important factors include being single-especially if a person has never been married. Whites and African Americans are more likely to be in nursing homes than Asians and Latinos, although other work has found that the gap has been shrinking over recent decades.12 In addition, women are more likely to live in nursing homes than men, but that is primarily because they live longer, have more self-care limitations, and are more likely to be unmarried (or widowed). Once we control for these factors, men are slightly more likely to be in nursing homes.
Planning for the future
We have shown that the number of seniors requiring support to live at home, and the number requiring nursing home care, will increase significantly by the year 2030. In the near future, California policymakers can anticipate a demand for increased spending on programs like Medi-Cal and In-Home Supportive Services (IHSS). Policymakers should also plan for the efficient use of state resources and incorporate the specific wants and needs of this generation of seniors. To do so, it is helpful to think in two broad categories: where seniors will live, and what type of workers they will need for help. In this section, we touch briefly on these two issues.
The state can anticipate that most seniors will prefer to remain in their own homes for as long as possible. California pays 50 percent of Medi-Cal costs, which include both IHSS services and nursing home care. Nursing home care is considerably more expensive than home- and community-based services and IHSS support. In 2015, a semi-private room in a nursing home costs 68 percent, or nearly $30,000, more than 40 hours a week of support from a home health aide.13 From a budgetary perspective, the state should implement regulations that reserve nursing home care only for those whose needs cannot be supported in their own home.
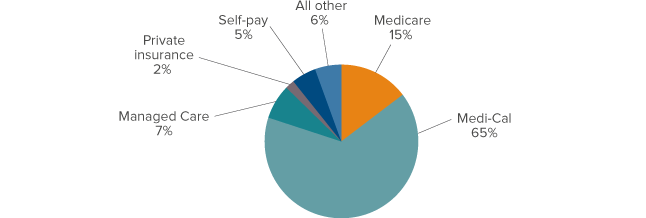
Figure 6. Medi-Cal is the primary source of funding for nursing home residents
SOURCE: California Office of Statewide Planning and Development, 2013.
NOTE: Medi-Cal spending is split evenly between California and the federal government. Medicare is federally funded. Managed care refers to health delivery systems that coordinate care across providers in an effort to improve efficiency and control costs.
Policymakers will also need to consider workforce development in anticipation of the growing senior population. The source, location, and type of care provided all determine the types of workers seniors will rely on. While there will certainly be a need for more doctors and nurses, the biggest demand for workers will occur in allied health professions, such as physician’s assistants, medical assistants, and home health aides. In addition to working in traditional medical settings, these workers will be especially important in providing home- and community-based services. Previous PPIC work has explored the state of California’s allied health workforce and training programs, as well as options to meet workforce needs in the future (McConville, et al. 2014). This work suggests that California policymakers can most effectively address the state’s health workforce needs through the community college system and programs that increase access and funding for postsecondary education.
In addition to addressing the sheer number of workers needed, state policies and programs should also bear in mind the increasing diversity of seniors. As we saw, the ethnic and racial makeup of the over-65 population is going to change significantly. Even within broadly defined racial and ethnic groups there are important cultural differences. With that in mind, it will be important to ensure that the growing health workforce is culturally competent.14 The state can address this issue both by supporting outreach, education, and training for workers across racial and ethnic groups, and through the IHSS program, which would allow participants to hire support workers from their own family or community.
Conclusions
California’s senior population will grow rapidly over the next two decades, increasing by an estimated 87 percent, or four million people. This population will be more diverse and less likely to be married or have children than seniors are today. The policy implications of an aging population are wide-ranging. We estimate that about one million seniors will have some difficulties with self-care, and that more than 100,000 will require nursing home care. To ensure that nursing home populations do not increase beyond this number, the state will need to pursue policies that provide resources to allow more people to age in their own homes.
There are many policies that could push the state toward that goal. The IHSS program provides resources for seniors to hire workers, including family members, to provide support with personal care, household work, and errands. One benefit of hiring family members is that they may provide more culturally competent care. Medi-Cal is already the primary payer for nursing home residents, and the state could potentially save money by providing more home- and community-based services that support people as they age, helping to keep them out of institutions. Finally, the projected growth in nursing home residents and in seniors with self-care limitations will require a larger health care workforce. California’s community college system will be a critical resource in training qualified workers focused on the senior population.
While this report provides projections for the year 2030, the issues of California’s growing senior population are important today. The oldest Baby Boomers are now in their late 60s, and this group will require increasing levels of services and support in the immediate future. In this report, we have focused on 2030 as a critical point in managing a new, larger number of seniors in the state. But California should anticipate that its aging population will require a range of policy responses before that time to address both short- and long-term challenges.
Topics
Health & Safety Net Population

